Why I no longer believe in annual health check ups
Our proactive health research reveals why a once in a year measurement misses the signals that matter most.

From an early age and like many, I have found the occasion of that trip to the local surgery for the annual (ish) check-up somewhat distressing. I’m not sure if it’s that unsettling disinfectant smell, soulless waiting room or the uncertainty that comes with someone unfamiliar checking you over and running tests that leaves me in a cold sweat. Probably a combination of all the above to be fair and an unhealthy dose of hypochondria thrown in for good measure no doubt. However, this has reliably informed the well documented phenomenon of a spike in my blood pressure. Now in the traditional check-up model, context rarely features in the results and for years this single moment of measurement has carried a disproportionate amount of weight for me.
Then in early 2020, pre-Covid, I was introduced to continuous health technology, wearables that track physiological signals across days, weeks and months not just minutes. For the first time, I could see what my body looked like outside the doctor’s surgery. My base lines emerged with visible variability and short-term spikes stopped being mistaken for longer term trends. That shift completely changed my understanding of health data and how seriously I take once a year measurement in isolation.
The point here is not my blood pressure, but that context transforms data and without it even the most accurate measurements can mislead.
We decided to examine this gap properly and commissioned through our research arm, Atomik Research, a nationally representative study of 3003 UK adults balanced by gender, spanning ages 18 – 65 and reflective of the UK’s socioeconomic profile. The aim was to interrogate the structural healthcare hypothesis.

Are we measuring health in a way that reflects how people live?
The results were revealing.
On the surface, engagement appears strong. 91% of Brits say they go to the GP with 45% going onto say they visit regularly.
But beneath that, the day-to-day reality tells a different story.
51% of Brits get 6 hours of sleep or less per night.
28% say they rarely or never sleep sufficiently.
63% experience stress regularly with 13% feeling it daily.
These are not occasional health events; they are recurring physiological inputs.
And yet monitoring remains low.
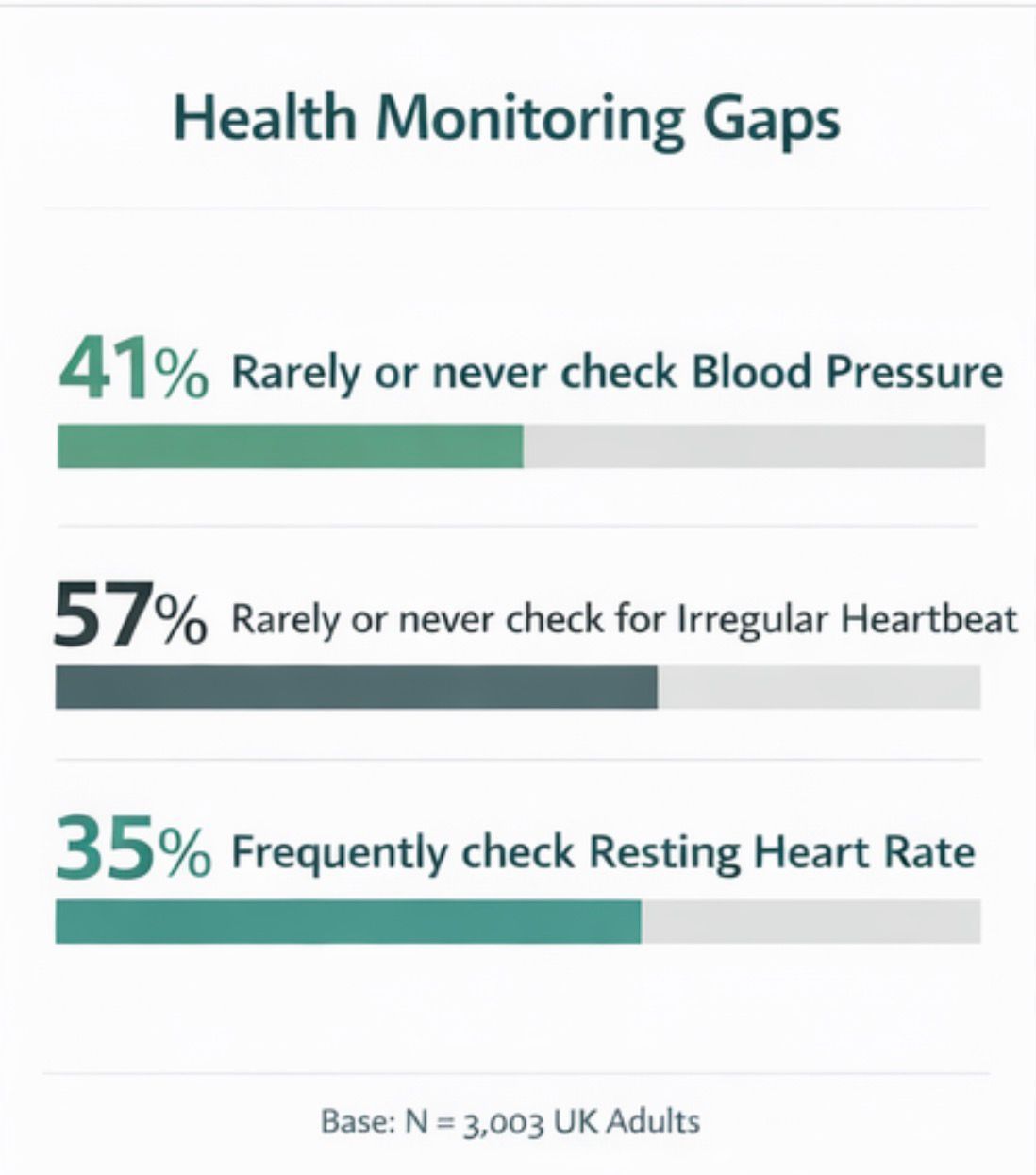
41% rarely or never check their blood pressure.
57% rarely or never check for irregular heartbeat.
Only 35% frequently check their resting heart rate.
We are living in bodies that generate continuous signals but most of us are not observing them. The disconnect becomes even clearer when looking at behaviour verses intention.
Brits want longevity. On average, people say they’d like 25 additional healthy years. 75% are confident they’ll live long lives.
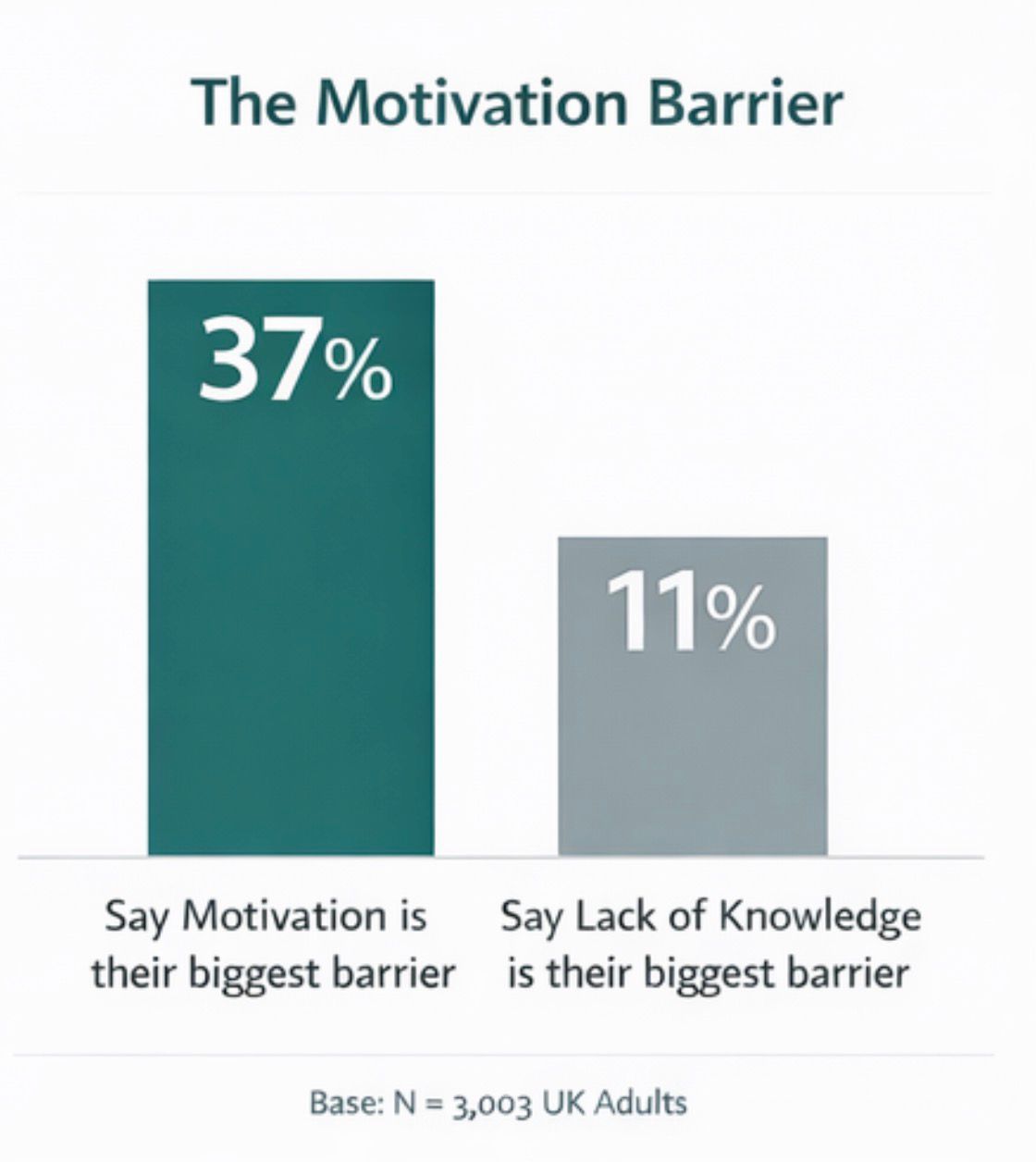
But 44% are already worried about their future health and when asked what stands in their way, 37% cite motivation compared to just 11% who say knowledge is the barrier. This is not an awareness problem, it’s an activation problem.
And that’s where cadence matters. Among the 34% already using health wearables with a further 38% open to them, behaviours shift noticeable.
87% say wearables improve their motivation to stay healthy. 43% say they do so “very much”.
The difference is not access to doctor’s; it’s the feedback frequency.
When people can see their sleep debt increasing, their resting heart rate trending upwards or their recovery faltering, behaviour becomes tangible. Without that feedback, health remains abstract, something to worry about annually rather than taking ownership and managing daily.
Perhaps most tellingly, 39% rarely or never think about longevity in daily life and 45% never consume longevity focused content. There is both a motivational gap and an educational white space.
We have built a healthcare system that intervenes episodically, but we are living in a culture increasingly aware of longevity yet under equipped to operationalise it.
This is the structural tension piece.
The annual check-up isn’t wrong, its incomplete.
It answers, “where are you today?” but proactive health asks “where are you drifting?” Drifting is where most of the long-term outcomes are shaped.
For brands, insurers, health tech innovators and employers this gap is commercially and culturally significant. The demand signals are there, 72% are open to wearable tracking, 56% already use supplements, younger people are entering the longevity market early. But motivation, monitoring and behaviours remain underdeveloped.
Understanding that gap between optimism and action, access and activation is precisely what this study set out to explore.
When 91% engage with healthcare, yet half of the country is sleep deprived and two thirds experience regular stress, this issue is not awareness. Its alignment.
When I said at the beginning that I no longer believe the annual check-up reflects how health actually works, I didn’t mean it dismissively. I meant it structurally. Health is continuous and our measurement models largely are not. The data doesn’t suggest abandoning doctors it suggests expanding the feedback loop between appointments. The real opportunity isn’t replacing annual moments it’s reducing the drift between them.
We help brands uncover the truths that shape strategy. Get in touch to see what best in class Atomik Research looks like.